By Lt. Gen. Ronald R. Blanck, USA (Ret), Vice Adm. Harold Koenig, USN (Ret), and Lt. Gen. Charles H. Roadman II, USAF (Ret)
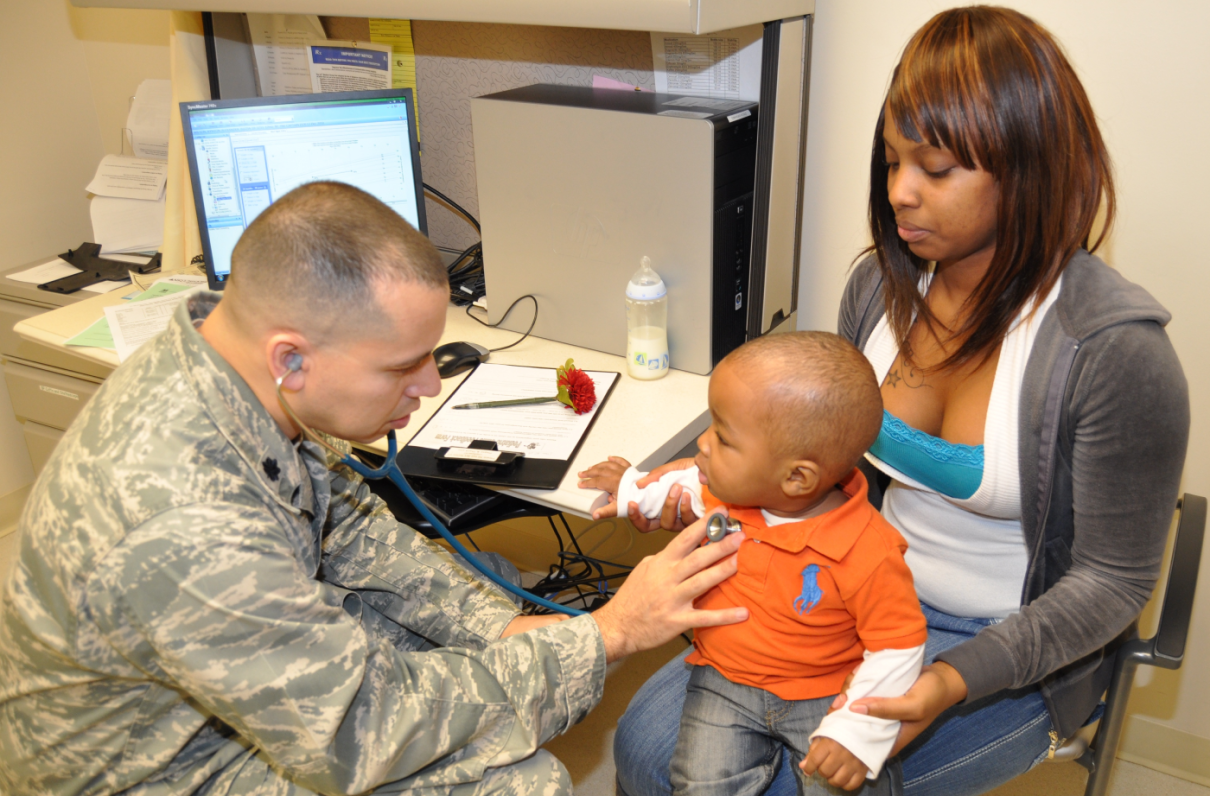
Military medicine’s responsibility is to keep soldiers, sailors, airmen, and Marines healthy so they can deploy and fight, to provide lifesaving medical care on the battlefield and rehabilitate service members after they are wounded. Military medicine’s success has reduced the percentage of troops who have died of battlefield wounds to a historic low for the most recent two longest wars in American history. Death casualties have fallen steadily from nearly 20% in World War II to 17% during the Vietnam conflict to below 9% now.
Since the end of the draft in 1972, this has been accomplished by operating Graduate Medical Education programs in our largest military hospitals. These programs have provided a steady supply of well-trained military physicians, nurses and other health professionals.
[TAKE ACTION: Ask Your Lawmaker to Protect Military Medicine]
Military hospitals and clinics are also platforms for on-the-job and sustainment training for our enlisted combat medics who are the first responders on the battlefield. Military hospitals also provide care to family members, eliminating the worry from warfighters that their family members will not receive needed care during their absence. In addition, medical research relevant specifically to the military, but not necessarily the civilian population, is also carried out.
Congress believes there are efficiencies to be gained by reorganizing the existing Army, Navy, and Air Force medical systems into a single tri-service medical agency. While this major reorganization moves forward, the Department of Defense, at the recommendation of Pentagon budgeteers and the three services, has taken the opportunity to propose personnel cuts of as much as 20% in the military medical departments.
This would significantly degrade military medicine’s current capabilities and threaten its ability to carry out its core missions.
As former Army, Navy, and Air Force surgeons general, we strongly assert the need for Congress to table these cuts until a thorough study of the potential consequences of these reductions are evaluated.
The risks of relying on what is, at best, a superficial analysis of promised cost savings derived from large-scale reductions will lead to reduced readiness by not having enough physicians, nurses and medics to care for those in war zones.
[RELATED: House Defense Bill Includes Pay Raise, Widows Tax Repeal]
Further, this short-sighted depletion of capability erodes the training base (graduate education and other programs that generate the medical force), relies on uneven or unavailable civilian care for family members, and will negatively affect recruitment and retention.
If even one of these “high-risk, high-regret” consequences unfolds, the percent of those dying from wounds will increase, the all-volunteer force will suffer, and we may be forced to again draft medical personnel – including physicians.
Retired Lt. Gen. Ronald R. Blanck was the Surgeon General of the Army from 1996-2000. Retired Vice Adm. Harold Koenig was the Surgeon General of the Navy from 1995-98. Retired Lt. Gen. Charles H. Roadman II was the Surgeon General of the Air Force from 1996-99.